
 (732) 246-1377
(732) 246-1377
 (732) 246-1377
(732) 246-1377
Cracked heels can make life very frustrating and embarrassing when displaying the bare feet. Aside from being unpleasing to the eye, they can also tear stockings and socks and wear out shoes at a faster rate. When severe, cracked heels may cause pain or infection.
Cracked heels are a problem for those who are athletic, those who may walk a lot, and those who have especially dry skin. Those who use medication that dry the skin, those who swim often, wearing certain types of shoes, and those who are diabetic may have trouble with cracked heels. Seniors whose skin produces less oil may also have trouble with cracked feet. There is no one way to develop cracked feet, and there is no cure.
Today, the market consists of numerous products that have a variety of ingredients to promote healing. Some of these are over-the-counter. Others are prescribed by a doctor, especially for those who have chronic dry feet and heels.
Some doctors recommend wearing socks at night for those with rough skin. This helps further healing, and helps creams stay on longer and better absorb into the skin.
One way to alleviate dryness that causes cracked heels is by using moisturizers both day and night. Another way is to make sure the skin is clean and dry at all times. Using a pumice stone to buff away dead skin before putting on moisturizer can also help. Cracked heels will not respond to the cream unless the outer layer of skin is first removed through exfoliation. After exfoliation, lotion or ointment will be absorbed by the skin more easily.
Foods that produce healing and balance can also help the skin from within. Everything that is put into the body can either help it or hurt it. Taking supplements of omega-3 fatty acids and zinc can also be very beneficial.
Nevertheless, not all products are guaranteed to help treat cracked feet. Seeing a professional is best if other treatments options were unsuccessful. A podiatrist should be able to give the best advice to help with this problem.
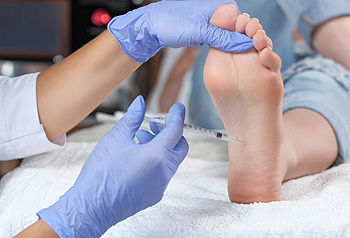 The ankle-brachial index (ABI) is a quick and non-invasive form of vascular testing that your podiatrist may perform during a routine visit. It is frequently used to assess the presence or severity of peripheral artery disease, a potentially dangerous condition that results in poor circulation to the lower limbs. The ankle-brachial index test is performed in several steps. Similarly to typical checkups at your physician’s office, first, the doctor will measure your blood pressure around your upper arm. Then, the doctor will measure your blood pressure around your ankle. The two numbers are compared to find the ankle-brachial index value, a number that is used to determine the presence or severity of peripheral artery disease. The lower the ABI value is, the greater the chance that you have arterial disease. If you suspect you have poor circulation to your lower limbs, it is recommended that you visit a podiatrist, who can perform an ankle-brachial index test, as well as other vascular tests to assess blood flow to your feet and ankles.
The ankle-brachial index (ABI) is a quick and non-invasive form of vascular testing that your podiatrist may perform during a routine visit. It is frequently used to assess the presence or severity of peripheral artery disease, a potentially dangerous condition that results in poor circulation to the lower limbs. The ankle-brachial index test is performed in several steps. Similarly to typical checkups at your physician’s office, first, the doctor will measure your blood pressure around your upper arm. Then, the doctor will measure your blood pressure around your ankle. The two numbers are compared to find the ankle-brachial index value, a number that is used to determine the presence or severity of peripheral artery disease. The lower the ABI value is, the greater the chance that you have arterial disease. If you suspect you have poor circulation to your lower limbs, it is recommended that you visit a podiatrist, who can perform an ankle-brachial index test, as well as other vascular tests to assess blood flow to your feet and ankles.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with one of our podiatrists from Livingston Footcare. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our office located in North Brunswick, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
 Warts, which can grow throughout the body, are outgrowths on the skin that are caused by human papillomavirus (HPV). Warts can be very contagious, and they can spread through skin-to-skin contact or through sharing personal items. Plantar warts grow on the bottom of the feet and usually have tiny black dots in them. Generally, warts disappear over time, but it may take months for them to do so. While plantar warts are usually harmless, they can be very painful. There are a variety of treatment options for warts that are causing pain, including chemical treatments and lasers. Some podiatrists may even elect to surgically remove warts that have become a problem. If you are experiencing painful plantar warts, make sure to discuss with a podiatrist which treatment options may be right for you.
Warts, which can grow throughout the body, are outgrowths on the skin that are caused by human papillomavirus (HPV). Warts can be very contagious, and they can spread through skin-to-skin contact or through sharing personal items. Plantar warts grow on the bottom of the feet and usually have tiny black dots in them. Generally, warts disappear over time, but it may take months for them to do so. While plantar warts are usually harmless, they can be very painful. There are a variety of treatment options for warts that are causing pain, including chemical treatments and lasers. Some podiatrists may even elect to surgically remove warts that have become a problem. If you are experiencing painful plantar warts, make sure to discuss with a podiatrist which treatment options may be right for you.
Plantar warts can be very uncomfortable. If you need your feet checked, contact one of our podiatrists from Livingston Footcare. Our doctors will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact our office located in North Brunswick, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
Have you ever gotten up from a chair or out of bed in the morning, and upon taking that first step, feel like your heel has stepped on a tack? Many people experience a feeling of sharp pain which radiates into their arch from their heel and which does not allow them to put their heel on the floor. Sometimes they need to sit back down, stand only on their toes and use the wall for balance. If you can take a few steps, it seems to go away and lessen, allowing you to then resume your activity. Later, throughout your day and after a period of rest, it can happen again. If this sounds familiar you may be suffering from your first attack of heel pain.
Heel pain is a debilitating condition that affects day to day activities. Running and walking both causes stress on the heel because the heel is the part of the foot that hits the ground first. This means that the heel is taking on your entire weight. Diagnosis and treatments for heel pain can be easily found through your podiatrist.
Plantar Fasciitis
One of the main causes of heel pain is a condition known as plantar fasciitis. The plantar fascia is a band of tissue that extends along the bottom of the foot, from the toe to the bottom of the heel. A rip or tear in this ligament can cause inflammation of these tissues, resulting in heel pain. People who do not wear proper fitting shoes are often at risk of developing problems such as plantar fasciitis. Unnecessary stress from ill-fitting shoes, weight change, excessive running, and wearing non-supportive shoes on hard surfaces are all causes of plantar fasciitis.
Achilles Tendonitis
Achilles tendonitis is another cause of heel pain. Similar to plantar fasciitis, inflammation of the Achilles tendon will cause heel pain due to stress fractures and muscle tearing. A lack of flexibility of the ankle and heel is an indicator of Achilles tendonitis. If left untreated, this condition can lead to plantar fasciitis and cause even more pain on your heel.
Heel Spur
A third cause of heel pain is a heel spur. A heel spur occurs when the tissues of the plantar fascia undergo a great deal of stress, leading to a separation of the ligament from the heel bone entirely. This results in a pointed fragment of bone on the ball of the foot, known as a heel spur.
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Your feet endure a great amount of stress each day from constantly allowing us to move around. It is important to stretch your feet to help prevent them from becoming injured. Your toes may easily deform into unhealthful positions if they are not stretched.
One of the most common reasons for toe deformities are the shoes you may be wearing. Shoes that are too tight may fold and shift the toes out of place. Heeled shoes may also push your toes upward. Forcing your toes into an unnatural position which may cause the muscles to tighten and prevent them from reverting to normal length. Another common reason is improper use of foot muscles. Many people fail to use the muscles in their feet or toes when they walk. Lastly, the positioning of your feet while walking may also cause toe deformities. If you walk with your feet facing outward, your “push-off” phase is on the side of your big toe instead of the bottom of your foot. This may cause the big toe to eventually tighten into a new shifted position.
There are many reasons why stretching your toes may be helpful. One reason is that healthy spacing may aid in avoiding calluses and other injuries that are caused by rubbing. Stretching will also prevent you from developing toes that curl, hammertoes, or bunions.
A great way to stretch your toes is to place them in your hands and bend them all downward; this will help you stretch the top of your foot. Next, you should repeat this process but instead bend them upward enough to feel a nice stretch in the bottom of your foot. You should then try to pull each toe apart from the next and pull any toes that are bent upward until they are back downward.
If you are looking to practice stretching your entire foot, you can try a towel stretch. This is done by sitting on the floor with your legs in front of you. Take a towel and wrap it around your toes. Afterward, pull the towel toward you with your toes and hold this position for 15 to 30 seconds before releasing. Practice this stretch for three sets. Another stretch your feet are towel lifts. This is done by sitting in a chair and trying to pick a towel up from the ground with your toes. Try lifting the towel with your little toes for five sets before switching feet.
If you are an athlete, or exercise often, it is especially important for you to practice stretching your feet. Those who suffer from foot pain caused by poor footwear, plantar fasciitis, or long hours of standing at work may also benefit from foot exercises.